Bugged Out. Gross!: Identifying and Treating Four Childhood Diseases
The Down and Dirty Facts About Four Easily Spread, Icky Childhood Diseases.

Put your child with a group of kids and he or she will inevitably catch something that makes you squirm. The symptoms are usually worse than the ailment and the bugs easy to treat.
Pinworms, ringworm, impetigo and hand, foot and mouth disease are communicable diseases with visible, unpleasant symptoms. Use this guide to identify, get rid of and prevent the culprits from returning.
Say What?
A communicable disease is highly contagious or infectious, and spreads easily from person to person.
“There is an unfair stigma associated with many common infectious diseases,” says Dr. Brian Tanabe, pediatric and adolescent medicine specialist at Straub Family Health Center. “Children who contract these diseases do not necessarily have poor hygiene or care. All kids are susceptible,” he says.
Returning to School
Lory Gaskill, Mid-Pacific Institute’s middle- and high-school nurse, advises parents to check with their children’s schools when a diagnosis is made. Policies differ among schools, and according to the ailment.
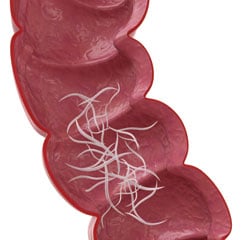
Pinworms
What They Are
Pinworms are white (almost clear) parasitic worms the size of a staple. Children ingest microscopic pinworm eggs by putting their hands or fingers in their mouths after touching an object or surface that was touched by someone with pinworms. The eggs hatch in the intestines, then the females travel out of the body through the anus to lay more eggs.
When children scratch their itchy bottoms, the eggs get under their fingernails and are easily spread to other surfaces, where they can survive for two to three weeks.
How to Diagnose
The females tend to lay their eggs in the evening. Children may complain of tummy aches or pain and itchiness near their bottoms. They may squirm uncomfortably and have trouble falling asleep. Small children have a hard time identifying the discomfort, and their only symptom may be crying or fussiness.
When your child is asleep, check the anus area for worms. “If worms seem hard to detect, apply clear scotch tape to the anus, then place the tape on a glass slide. Your doctor or the lab can view the slide to confirm the presence of eggs. However, the clinical picture is often enough to make the diagnosis,” says Tanabe.
What to Do
Let your child sleep. In the morning, wash the infected area, hands and fingernails, and bedding, clothing and towels.
Contact your doctor for a prescription anti-worm medication or an over-the-counter option. He or she may suggest treating the entire family. The medication should be repeated in two weeks.
How to Prevent Them
- Remind children to wash their hands after playing, coming home from school, using the bathroom and before eating.
- Bathe and change underwear daily.
- Trim and clean fingernails regularly.
- Remind children not to scratch their bottoms and/or bite their nails.
One Honolulu mom, whose daughters, 6 and 8, have had pinworm infections off and on since they were 3, reminds her children often to wash their hands and keep their fingers out of their mouths, but they don’t always do it. “We always have a bottle of ‘PinX’ on hand, just in case,” she says.

Ringworm
What It Is
Ringworm is a fungal infection—not a worm—of the skin that thrives in warm, moist areas. Kids can catch it from other children, animals and soil. “We often see high-school athletes in contact sports like football and wrestling with this infection. Occasionally, their younger siblings also get infected, presumably from close household contact,” says Tanabe.
How to Diagnose
An infection on the scalp causes hair loss, leaving itchy, round, red patches. Skin infections, which can occur anywhere on the body, become scaly and red. Ringlike lesions with raised borders and clear centers, between the size of a dime and a quarter, may develop. Without treatment, the lesions may become large. Usually, no testing is necessary for your doctor to confirm the diagnosis.
What to Do
The infection can be treated with prescription oral or topical antifungal medications or over-the-counter creams, which heal it within two to four weeks.
How to Prevent It
Teach your children not to share hats, brushes, other hair care products and towels. Avoid contact with infected children or animals. Wash hands well and shower soon after sporting events and practices.
Impetigo
What It Is
Impetigo is a skin infection that occurs when staph or strep bacteria enter the skin, usually at the site of an existing problem, such as eczema, bites or cuts. It is most often around the nose, mouth, hands, forearms and diaper area.
How to Diagnose
Doctors examine the appearance of the rash, sometimes sending a sample of fluid from the blisters to a lab. There are two types of impetigo:
Type One: Bullousimpetigo (large blisters), caused by a bacteria that releases toxins which trigger the formation of large, fluid-containing blisters that are first clear, then cloudy.
Type Two: Non-bullous impetigo (crusted) impetigo is the most common. It begins as tiny blisters that eventually burst and leave small, wet patches of red skin which may weep fluid. Gradually, a tan or yellowish-brown crust covers the affected areas.
What to Do
When a small area of the skin is affected (especially with the non-bullous form), it can be treated with antibiotic ointment. If it has spread, or the ointment isn’t working, the doctor may prescribe an antibiotic pill or liquid.
With treatment, healing should begin within a few days. It’s important that your child takes the medication as prescribed, or a deeper, more serious infection could develop.
While healing, wash infected areas daily with clean gauze and antiseptic soap. Soak areas of crusted skin in warm, soapy water to remove the layers of crust (it is not necessary to remove it all).
To keep impetigo from spreading, cover infected areas with gauze and tape or a loose plastic bandage. Clean and trim your child’s fingernails.
How to Prevent It
Practice good hygiene and tend carefully to cuts, scratches, rashes and bites until the skin is no longer compromised.
Hand Foot and Mouth Disease (HFM)
What It Is
Hand, foot and mouth disease is a virus that lives in the body’s digestive tract and spreads from person to person, usually on unwashed hands and surfaces contaminated by feces. Kids ages 1 to 4 in childcare or preschools are most prone to the disease, which typically lasts three to five days.
How to Diagnose
Children develop painful blisters in the throat, tongue, gums, hard palate or inside the cheeks. Blisters are red, with a small bubble of fluid on top, and often turn into ulcers. The soles of the feet and palms of the hands may also be affected with a rash that looks like flat, red spots or red blisters.
Occasionally, a pink rash may be seen on other parts of the body, such as the buttocks and thighs. Some children with HFM may only have the sores in the back of the throat and mild symptoms.
It can be hard to detect HFM if sores are only inside the mouth or throat. Very young kids may not be able to complain of a sore throat, but if they stop eating or drinking, or want to eat or drink less often, it’s a signal that something is wrong.
A child also might:
- Develop fever, muscle aches or other flulike symptoms
- Become irritable or sleep more than usual
- Begin drooling (due to painful swallowing)
- Gravitate toward cold fluids
What to Do
There is no vaccine for HFM. Hand washing is the best protection. Remind everyone in your family to wash their hands frequently.
Keep kids home from school and childcare while they have a fever or open blisters on the skin and mouth.
Acetaminophen or ibuprofen can be given to console an achy or irritable child. Cold foods such as ice cream and popsicles can ease throat pain.
Blisters on hands or feet should be kept clean and uncovered. If a blister pops, dab on antibiotic ointment to prevent infection and cover with a small bandage.
Your child should drink plenty of fluids to prevent dehydration.
How to Prevent It Good hygiene and effective hand washing are paramount.








